Official Journals By StatPerson Publication
|
Table of Content - Volume 11 Issue 1 - July 2019
Effect of screw neck angle and screw parallelism in fixation of fracture neck of femur by partially threaded cancellous screws
Lakshya Prateek Rathore#, Mukand Lal$, Sandeep Kashyap*
#Senior Resident, Department of Orthopaedics, SLBS Government Medical College and Hospital, Mandi at Near Chowk, Himachal Pradesh. $Professor and HOD, Department of Orthopaedics, IGMC Shimla, Himachal Pradesh, INDIA. *Assistant Professor, Department of Orthopaedics, IGMC Shimla, Himachal Pradesh, INDIA. Email: dr.lakshya.rathore@gmail.com
Abstract Aims: The objective of this study was to investigate and evaluate the effect of screw parallelism and neck screw angle on functional outcome and prognosis of femoral neck fractures in young adults ficed closed with Partially Threaded Cancellous Screws (PTCS). Patients and methods: Here are presented 64 patients, both retrospective and prospective who were treated with closed reduction and internal fixation with PTCS. Ages of the patients ranged from 18-59 years. The patients were followed up for a minimum period of one year and the functional results were assessed with the help of modified Harris hip score and the Oxford hip score. Apart from general complications, the study was focussed on the two most dreaded complications of fracture neck femur, osteonecrosis and non union. Results: Most of the patients with parallel (90.7%) and divergent (68.8%) configuration of screws had excellent to good scores. 90.6% of the patients with parallel screw configuration and 87.5% of the patients with divergent screw configuration did not develop osteonecrosis. Both these correlations were found to be significant (p value <0.05). similar results have been seen with screw neck angle, a new parameter which has not been used before in any of the studies available in the literature. Conclusion: The role of screw parallelism and neck screw angle in predicting functional outcome and guiding the treatment is significant and needs further investigation to reaffirm its role in the same.
INTRODUCTION Hip fractures are common and comprise about 20% of the operative workload of an orthopaedic trauma unit. Intracapsular femoral neck fractures account for about 50% of all hip fractures1.Femoral neck fractures have all the problems associated with healing of intracapsular fractures elsewhere in the body. The portion of the femoral neck that is intracapsular has essentially no cambium layer to participate in peripheral callus formation in the healing process2. Therefore, healing in the femoral neck area is dependent on endosteal union alone3, which is one of the reasons that prolonged union times are commonly seen in these fractures. Unless the fracture fragments are carefully impacted, synovial fluid can lyse the blood clot formation4 and thereby destroy another mode of secondary healing by prevention of formation of cells and scaffolding that would allow for vascular invasion of the femoral head. In 1960, Claffey concluded that in all femoral neck fractures that communicate with the point of entry of the lateral epiphyseal vessels, aseptic necrosis occurred5. In addition to the specific biology of the fracture healing and the typical vascularity of neck of femur, the displacement of the fracture fragments can render them avascular. Hence survival of the femoral head and fracture union is largely dependent on preservation of what is left of the blood supply. Union can still occur through some avascular fragments also but it is prudent to that an accurate and stable reduction is achieved.6 In the young adult, that is less than 60 years of age, the preferred treatment is internal fixation while in elderly it is total or hemiarthroplasty7. There is little consensus in the literature regarding the optimal treatment of this injury, although its vastly believed that other than injury and displacement factors, the fracture reduction, posterior comminution and implant positioning is very important8. Commonly used implants for fixation are partially threaded cancellous screws (PTCS) or sliding hip screw (SHS)9. Also very recently Dynamic Locking Blade Plate (DLBP) has been used in a study by Kalsbeek et al in Netherlands and showed good results.10 Many surgeons prefer to use PTCS in the treatment of femoral neck fractures considering its many advantages like compression at fracture site, less voluminous implant, collapse-allowing etc. However, there seems to be a severe dearth of literature that details the radiological parameters that govern the optimal position of PTCS on the radiographs and their relative configuration in order to achieve a desirable outcome. In this study we aim to delineate various such parameters pertaining to PTCS in the closed reduction internal fixation of fracture neck of femur and hopefully give substantial evidence to their better use in the future.
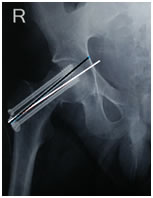
MATERIAL AND METHODS Study design: 39 retrospective and 25 prospective (total 64) cases that were treated by closed reduction internal fixation of fracture neck of femur at our institute in the last 6 years. Institutional ethical board approval was obtained for the same. Patient selection: patients in the age group of 18-59 years who had a fracture of the neck of femur and treated with closed reduction internal fixation with PTCS. Pathological fractures and fractures operated with open reduction were excluded from the study to reduce the confounding factors. Patients underwent surgery after complete work up and clearance from the anaesthesia department. Patients were discharged on the 5th day after 2 dressings on the 2nd and 5th day. Suture removal done on 14th day and patient allowed partial weight bearing with crutches on 6 weeks follow-up, whence forth 6 weekly x-rays were taken and weight bearing increased gradually. At each visit patients were assessed using both the Modified Harris Hip Score (HHS) and Oxford Hip Score (OHS). Radiological Assessment Screw neck angle was measured as the angle which the long axis of the neck of femur (whiteline) makes with the long axis of the screw (black line) in the anteroposterior x-ray view. It was calculated for each screw and divided into three groups based on the highest value obtained (figure 1). Figure 1 RESULTS Out of total 64 patients, the age ranged from 18-65 years with maximum age of 59 years and minimum of 18 years. Most of the patients were between the age of 40-59 years constituting more than 50% of the total population. The mean age in our study was 43.3±8.1 years. Maximum number of patients (82%) had a screw neck angle of less than 5 degrees. 18% of the patients had an angle more than 5 degrees. It was found in our study that patients with screw neck angle less than five degrees had a better outcome as compared with those who had screw neck angle more than 5 degrees and this correlation was found to be significant with a p value of 0.020 (table 1)Eighty two percent of the patients had a parallel arrangement of screws or were divergent. In 18% of patients, screws were convergent. Most of the patients with parallel (90.7%) and divergent (68.8%) configuration of screws had excellent to good scores. Significant correlation was found on comparison of screw parallelism with Modified Harris hip score with a p value of 0.047 (table 2). There were 5% cases of non union which did not show any significant results with any of the parameters under study. About ninety six percent of the patients with screws parallel to the neck did not have any signs of osteonecrosis while 75% of those with neck screw angle between 1 to 5 degrees did not have any osteonecrosis. This correlation between neck screw angle and the incidence of osteonecrosis was found significant with a p value of 0.019 (Table 3) 90.6% of the patients with parallel screw configuration and 87.5% of the patients with divergent screw configuration did not develop osteonecrosis. The correlation was found to be significant (p value 0.019) (Table 4). Table 1: Modified Harris hip score in relation to screw neck angle
Table 2: Correlation of Modified Harris Hip score with screw parallelism showing significant results
Table 3: Osteonecrosis in relation to screw neck angle
Table 4: Osteonecrosis in relation to screw parallelism
DISCUSSION REFERENCES
|
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
 Home
Home