|
Table of Content - Volume 21 Issue 2 - February 2022
In situ placement of ulnar nerve in distal humerus fractures with bicolumnar fixation and post operative incidence of ulnar neuropathy: A retrospective study
S Navin Chander1, A Senthilnathan2*, R Prabhakar3, K Parasuraman4, K Vijaya Shankar5
1Postgraduate Student, 2Professor & HOD, 3Lecturer, 4,5Assistant Professor, Department of Orthopaedics, Rajah Muthiah Medical College And Hospital, Annamalai University, Tamilnadu, INDIA. Email: ncnavinchandar@gmail.com
AbstractObjectives: To evaluate the incidence of post operative ulnar neuropathy following ORIF with Bicolumnar Fixation without anterior transposition of ulnar nerve. This retrospective study is also aimed at assessing the frequency and severity of ulnar nerve injury following the above said procedure. Design: Retrospective Study Description: A total of 33 patients were included in the study; with a mean age of 44.6 years and were reviewed at a mean period of 4 years following surgery. Medical records and Mcgowan grading for ulnar neuropathy was employed for subjective evaluation of Ulnar nerve affliction. Setting: Rajah Muthaiah Medical College and Hospital, Chidambaram Patients: 33 patients with Distal humerus fractures with Bicolumnar plating Intervention: All patients of distal humerus fractures underwent ORIF and bicolumnar fixation without anterior transposition of ulnar nerve. Main outcome measurements: The primary outcome was to analyse the incidence of Ulnar neuropathy following in situ placement of ulnar nerve during ORIF of Distal Humerus fractures. Secondary outcomes included a assessing the severity of ulnar neuropathy as per Mcgowan grading. Results: 3 patients experienced, which could be relatively regarded as, mild ulnar nerve affliction. The duration of surgery in all 3 patients exceeded 120 mins. Mean period for resolution of symptoms was at 4.5 months. Conclusion: Thus, this low proportion of ulnar nerve affection in our case series endorses ORIF with bicolumnar fixation without ulnar nerve transposition for distal humerus fractures as an admissible choice. Keywords: Fracture, ORIF, Transposition, Distal Humerus, McGowan, Ulnar Nerve.
INTRODUCTION With an estimated proportion of 2% of all fractures; distal humerus is not quite ubiquitous like other fractures.1 Yet, these fractures are difficult to manage. For good results, it is imperative that an acceptable anatomic reduction is achieved, satisfactory articular congruity is maintained and a stable internal bicolumnar fixation is done.2-6 From a surgeon’s perspective, the consensus amongst the majority is that distal humerus fractures could be best managed with bicolumnar fixation.7 This procedure necessitates the isolation of ulnar nerve and warrants its mobilisation to some degree; thus rendering it vulnerable and possibly predispose it to a significant risk for an iatrogenic injury.7 Nevertheless, it is noteworthy that the causative of an ulnar neuropathy could be ascribed to the initial trauma itself, operative procedure or during post operative rehabilitation.8–12 Literature review gives a ballpark figure of around 13% for post operative ulnar nerve neuropathy; nonetheless it could vary from 0-51%.3,7,13–19 Few authors are strong proponents for routine transposition of ulnar nerve7,13,16, 18, 20–24 while some vouch against it; advocating in situ placement in the epicondylar groove.3,14,19 The present study aims to investigate the incidence the post operative ulnar nerve dysfunction subsequent to Open Reduction and Internal Bicolumnar fixation of Distal Humerus Fractures without routine Ulnar Nerve transposition or mobilisation and better understand the same. Study design: It was designed as a retrospective study to assess the prevalence of post operative ulnar neuropathy following distal humerus fracture ORIF with no ulnar nerve transposition. Fractures were classified on the basis of preoperative images including CT scans in accordance with the AO (Arbeitsgemeinschaft für Osteosynthesefragen) classification system.25 The outcomes were categorized into primary and secondary. The primary outcome studied involves the rate of ulnar nerve neuropathy (any clinical findings of ulnar nerve transient or permanent sensory or motor signs or symptoms. The secondary outcomes include the severity of ulnar nerve dysfunction and the recovery rate. The severity of ulnar nerve neuropathy was appraised along the lines as proposed by the McGowan classification.26 All the patients were segregated into three grades consistent with McGowan classification [26]. Grade I indicates mild lesions with no apparent motor weakness of the ulnar intrinsics and paresthesia along the distribution of ulnar nerve; but with a slight sensory blunting. Grade II corresponds to intermediate lesions; wherein the interossei are weak and obvious wasting of muscles with moderate blunting of sensibility as well. Grade III could be defined as lesions with significant severity; with paralysis of interossei and the marked hypoesthesia. Eligibility criteria: Adult patients who were operated for distal humerus fractures with bicolumnar fixation with no ulnar nerve transposition during the mentioned study period were included in the study. The exclusion criteria were cases with history of preexisting ulnar nerve neuropathy prior to trauma and those with deficient documentation of pre operative and post operative ulnar neuropathy. Surgical techniques: The choice of approach depended upon the fracture pattern, surgeon’s competenece and his discretion. Surgical approaches included Olecranon Osteotomy, Campbell’s posterior approach, Midline Triceps Splitting aproach, Para Tricipital approach and Von gorder approach. Ulnar nerve was identified after a cautious proximal dissection along the medial border of triceps, along its course, isolated and protected as a standard customary practice using vessel loop during the entire duration of procedure. Ulnar nerve alongside the perineural soft tissue was lifted off from the medial intermuscular septum and the humeral metaphysis during the placement of medial plate to allow for it to slide underneath. At the end of the procedure, the nerve was then restored back behind the medial epicondyle. (Fig-1) The patients were immobilised in a posterior splint for a duration of 14 days and after removal, active exercises as tolerated by the patient were started while strengthening exercises and load bearing were initiated after 6 weeks. Data Source and Collection: The medical records of patients with Distal Humerus fractures who underwent ORIF with bicolumnar fixation between January 2014 - December 2021 at Rajah Muthaiah Medical College and Hospital, Chidambaram were sought and comprehensively reviewed with an emphasis pertaining to Ulnar nerve - its intraoperative management and perioperative as well as postoperative function. Age, sex, mechanism of Injury, Open/closed fractures, fracture type according to the OTA/AO classification, time to surgery, surgical approach employed, duration of procedure, and the choice of implants used were also recorded.
RESULTS Participants: A total of 41 patients were identified following a broad and complete search of our institution database for patients who had undergone ORIF with bicolumnar fixation without ulnar nerve transposition during the mentioned study period. Out of which 5 patients were deceased and 2 could not be reached out due to their relocation elsewhere. One patient with prior history of ulnar nerve affliction preinjury was excluded. This left us over with a total sample size of 33 eligible patients; who were then contacted, offered and provided with follow up. Without exception, all were available for review and all of them participated in the follow up. Also, all were compliant. A minimal cut off criterion of 12 months and the maximum of 7 years was kept for post operative follow up period. Descriptive data: The study population showed a male predominace; 19 were females and 14 were males. The average age of patients was 47 years and the mean period of follow up was 4 years. Majority (20) gave a history of high velocity trama while the remaining gave a history of self fall (9), assault (2), fall from height (1) and sports injury in (1) patient. The exposure included an Olecranon osteotomy in 10 patients, Campell’s posterior approach in 10 patients, a Mid-line triceps split in 7 patients, Para tricipital approach in 4 patients and TRAP in 1 patient and Von Gorder approach in 1 patient. In reference to the AO classification, 12 fractures were type C1, 11 type C2, and the remaining 10 type C3 fractures Out of the 33 patients, 3 (9.09%) patients had documented post-operative ulnar nerve neuropathy which corroborated with their medical histories, nerve conduction studies and electromyographic studies whereas the rest of 28 patients had clear documentation of intact postoperative neurological function. Of the 3 patients, 2 presented with ulnar nerve dysfunction in their non dominant limb (Left) and the remaining One patient presented at his Dominant Limb (right). (Fig-2) All the three patients had undergone ORIF with Olecranon Osteotomy. 2 cases were classified as Mcgowan Grade 1 and 1 case as Mcgowan Grade 2. Characteristically, all 3 of them had AO C3 type distal humerus fracture and had a duration of surgery in excess of 120 minutes. Thus the probable implication from this observation would be that a challenging fracture pattern demands a longer duration of surgery while also increasing the odds of ulnar nerve injury. Nonetheless, all 3 of them had complete resolution of symptoms at their final follow up. The mean period for total recovery was at 4.5 months.
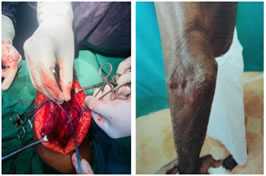
Figure 1 Figure 2 Figure 1: Insitu handling of ulnar nerve; Figure 2: Ulnar Neuropathy
DISCUSSION Ulnar nerve affliction usually presents with weakening of the hand grip along with paraesthesia over the ring and little fingers. This focal peripheral neuropathy is a well recognized phenomenon, with a retalively high prevalence, frequently seen after distal humerus fractures and is in itself a challenging complication despite the advancement in the treatment of distal humerus fractures. Ulnar nerve neuropathy has a varied etiology. The nerve is most liable to laceration or contusion during the initial trauma itself. Intraoperatively, the nerve is prone for inadvertent injury due to its fixed anatomic location, just behind the medial epicondyle, proves to be detrimental. The nerve is at greater risk for injury during its dissection and exposure, upon aggressive decompression, while manipulating the fracture fragments and implant placement. Hematoma formation during the immediate perioperative period might also induce an injury besides impeding its recovery as well. Heterotropic ossification, restricted terminal extension and scarring of the soft tissues; all effectuate and contribute to ulnar nerve injury while also hampering its recovery during the postoperative period. Retrospective evaluation done by Huang et al.27 in patients of distal humerus treated operatively had nil ulnar affliction following surgery. Comparable results were seen Doornberg et al.28 who claimed only a 3% incidence of postoperative ulnar nerve symptoms. Furthermore, Worden and Ilyas,29 demonstrated an incidence of a late ulnar neuropathy following ORIF at about 38%. In the present study, 9.09% of the patients operated with internal bicolumnar fixation of a distal humeral fracture reported symptoms from the ulnar nerve at a 4-year follow-up. All the five patients were resolved of their symptoms completely at a mean of 4.5 months. By convention, identification and isolation of ulnar nerve is a regular and mandatory practice during ORIF of distal humerus fractures; however, intraoperative handling differs widely. The issue of appropriate and best method for surgical handling of the ulnar nerve has been addressed in several articles. There is paucity of studies over the indications for transposition; with some recommending it in the event of preoperative palsy, during possible intraoperative traction, on implant irritation following bicolumnar fixation extending into medial epicondyle while on the contrary some authors favor routine transposition; whilst few perform transposition citing no particular reason. Thus there exists an apparent controversy over indications to transpose. Although, some studies do exist which deem transposition to be beneficial in cases with preoperative palsies. The most feasible explanation to prefer transposition is that it eventually results in the ulnar nerve being kept away from the proximity of soft tissue edema, fracture inflammation, callous formation and periarticular fibrosis as well thereby inherently reducing its tension along its course. In all likelihood, these arguments influence some authors who routinely prefer to transpose the ulnar nerve in all cases. Having said that, transposition involves excessive nerve handling, a possible devascularization and a iatrogenic traction injury as a consequence. Also, incidences of late compressive neuropathy is a familiar occurrence due to poor and deficient decompression of soft tissue restraints in transposition. Wang and colleagues [13] reviewed 20 patients with intracondylar distal humerus fractures managed with bicolumnar plating and anterior subfascial ulnar nerve transposition by way of Olecranon osteotomy and established none amongst them to have postoperative nerve compression symptoms during the follow-up period. Ruan et al.,11 reported superior results in patients of distal humerus fractures with preoperative ulnar nerve dysfunction when followed with transposition than those managed with in situ decompression. Likewise, McKee et al.,30 too echoed similar observations from his study; wherein he performed ulnar nerve transposition in 21 patients with ulnar nerve dysfunction following elbow surgeries and achieved good to excellent outcomes in 17 patients. Consequently, they hypothesized that transposition could be advantageous as it showed to be beneficial in recovery of nerve function post operatively. Gofton and colleagues7 credited routine transposition for the low incidence of objective ulnar neuropathy. Nevertheless, routine transposition in itself might result in post operative development of ulnar neuropathy as evident from studies done by Athwal et al.31 Their studies put a prevalance rate of post operative ulnar neuropathy around 13%. According to a study by Shin and Ring [18], regardless of sufficient release and transposition, incidence of post operative ulnar nerve palsy was pegged around 22% while upto 50% showed transient sensory symptoms. Worden and Ilyas29 and Vazquez et al.12 as deduced from their studies; concurred that ulnar nerve transposition offered no significant benefit over in situ decompression in minimizing the incidence of ulnar neuropathy. Additionally, Vazquez et al.12 calculated an occurence rate of 16% for iatrogenic ulnar dysfunction irrespective of procedure. Irrespective of whether an Ulnar nerve transposition was done or not, an incidence of ulnar neuropathy at 16% was observed by Wiggers et al.19 Meanwhile, Chen et al. [32], described a four times incidence of ulnar neuropathy following transposition; thereby concluding that patients with routine transposition are prone for higher risk of ulnar neuritis. A randomized trail of ORIF vs Total Elbow Arthroplasty for bicolumnar distal humerus fractures with routine ulnar nerve transposition in both cohorts that was done by Canadian Orthopedic Trauma Society revealed a 20% incidence of ulnar neuropathy postoperatively.5 Holdsworth and Mossad [14] documented a 51% rate of transient ulnar neuritis after an ulnar nerve transposition. Besides, studies by McKee et al. [5] indicate a 20% incidence of ulnar neuropathy following identical procedure. In contrast, it could be explicated that in situ release affords minimal nerve handling and thereupon reduced chances of a subsequent devascularization and a potential traction injury. Kundel et al.3 noted a 27% incidence of ulnar neuropathy after an insitu release of ulnar nerve was done. Despite careful scrutiny and analysis of the available literature, varying inferences are surmised; thereby requiring cautious interpretation and validation of the data. The contradictory nature of the specifics and unclear indications as to when to transpose, a standardized method during the intraoperative ulnar nerve management could not be elucidated. There seems a lack of clear consensus amidst surgeons and dearth of evidence in literature concerning optimal handling of the ulnar nerve during ORIF. Nonetheless, some authors advocate routine anterior transposition of the ulnar nerve as a prophylactic and preventive measure of ulnar nerve neuropathy in fractures of distal humerus. Ulnar nerve requires delicate handling lest it becomes vulnerable to injury. This study is impaired by several constraints. Primarily, the retrospective design confers several shortcomings to this study. The rationale of operating surgeons’ for selecting routine in situ management of ulnar nerve over transposition was not well described or documented. It is acknowledged that a possibility of selection bias to have crept due to the non systematic choice to do routine in situ placement. Another drawback involves plausible non differential bias; for instance misclassification of ulnar nerve affliction and the severity of the ailment as the accuracy of the data was strictly dependant on the hospital progress and follow up notes. Additional determinants, such as sparsity of distal humerus fractures; estimated to attribute an insignificant 2% of all fractures, severely dents from having a sufficiently large study population. Plus, we also could not correctly discern the exact time point since the symptoms begun to ameliorate. Further limitations include the inability and feasibility to gauge the measure of how gentle the nerve was handled, which invariably effect the chances of ulnar nerve dysfunction. Other confounding factors were not known to impact the risk of ulnar neuropathy. Lastly, all 3 patients of postoperative ulnar neuropathy had a long operating time in excess of 120 minutes and withal a AO type C3 distal humerus fractures; it can be veritably ascertained that duration of surgery and a complex fracture pattern to be influencing variables in determining the risk of injury. Also, after a long and exhaustive analysis of numerous studies incorporating the incidence of ulnar neuropathy following anterior transposition, it is reliably learnt that that routine anterior transposition is not necessary without a preexisting ulnar neuropathy prior to initial trauma. Our underlying presumptions too lie in the similar lines. Finally, from our observations, we reckon that in situ placement of ulnar nerve during ORIF of distal humerus fractures precludes critical injuries to the nerve along with affording surgical simplicity. The drasticaly lower severity and curtailed rate of ulnar neuropathy in our study sample strongly tilts the balance towards in situ management and we perceive it to being an efficient way to intraoperatively manoeuvre the ulnar nerve substantiating our beliefs.
CONCLUSION In conclusion, that despite a meagre sample size of 33, and on assumption that a reasonable average period of 4 years for follow up would suffice for detection of most late neuropathies; we are of the opinion that ORIF of distal humerus fractures without anterior transposition is undoubtedly desirabe over transposition. Future prospective and preferentially randomized controlled trials is needed to affirm the lesser degree of association of ulnar nerve palsies after in situ management in ORIF of distal humerus fractures.
REFERENCES
Policy for Articles with Open Access
|
|
 Home
Home