Official Journals By StatPerson Publication
|
Table of Content - Volume 3 Issue 1 - July 2017
Orthofix in management of compound tibia fractures – A prospective study
R Gokul Nath1*, A V Shabi2
1Sr. Resident, 2Sr Assistant Professor, Department of Orthopaedics, Govt Tiruvarur Medical College, Dr.MGR Medical University, Tamil Nadu, INDIA. Email: gokulmmc@gmail.com
Abstract Objective: Treatment of open tibia fracture is complex. Orthofix-Limb Reconstruction system can be used as definitive fixation of open tibia fractures with reliable results. Aim of this study is to evaluate outcome of the open tibial fractures treated with Orthofix. Method: The study is prospective study involving 30 patients with open Tibial fractures at our hospital. The patients were treated with wound debridement and stabilisation with Orthofix and followed up from August 2014 to April 2017. Then the patients were followed up to evaluate clinically, functionally by Lower Extremity Functional Score (LEFS) and radiologically by Radiographic union scale in Tibial fractures (RUST). Results: All the 30 patients included in our study had achieved bone union (100%).One patient (3.33%) had delayed union and required bone grafting and fibulectomy. The mean follow up period is 32.6 weeks. The average period taken for fracture union is 24.4 weeks. The mean LEFS score for the 30 patients at the end of follow up is 88.75%. The mean RUST score at the end of follow up is 2.6. Conclusion: Orthofix serves as external fixator and definitive fixation device as it allows dynamisation. Hence Orthofix is a very good device in Open tibial fracture management if proper rehabilitation measures and proper timing of dynamisation is followed. Key Words: Orthofix, Limb Reconstruction System, LEFS score, RUST Score, Compound Tibia fracture.
INTRODUCTION Tibial fractures are the most common long bone fracture, with approximately 25% being open1. The majority of open tibial fractures result from a high velocity trauma, such as a motorcycle accident. The treatment of open tibial fractures is complex because of lack of soft tissue coverage and blood supply of tibia. The outcome of the treatment is depended upon severity of comminution, degree of soft tissue injury, initial fracture displacement, and fracture reduction2. The main objectives of open tibia fracture management is to ensure soft tissue coverage of bone, eliminating infection, stabilising the fracture so as to help healing of soft tissue injury and hence helping in bone union, ultimately the functional recovery of patient The open fractures are classified based upon degree of soft tissue injury, amount of violence, level of contamination and fracture comminution. Two popular classifications for open fractures are Tscherne Classification and Gustilo-Anderson4,5 Classification. We have used Gustilo-Anderson Classification for open fractures to classify the fractures in our study. The options for treatment of open fractures are aggressive debridement of wound followed by internal fixation or by External fixation. Each treatment has its own merits and demerits. Primary internal fixation of open fractures in open fractures should be done in carefully selected group and that too after meticulous debridement3. Even after meticulous debridement, 10% of patients gone for deep seated infection and osteomyelitis in a study3. External fixation with recent advances like Ilizarov apparatus, Orthofix fixator the management of open tibia fractures by external fixation become more successful than past. MATERIALS AND METHODS The study is conducted at Govt Tiruvarur Medical College, The Tamil Nadu Dr MGR Medical University. The patients admitted with open tibia fracture are included in the study. In the study the open tibia fractures where managed by Limb reconstruction system Orthofix as definitive procedure. They are followed up to evaluate clinical, radiological and functional outcome. Totally 30 patients were included in this study. The period of study is from August 2014 to April 2017. The compound fracture is graded using Gustilo and Anderson Classification (Table-1). Implants Used The Orthofix used consists of
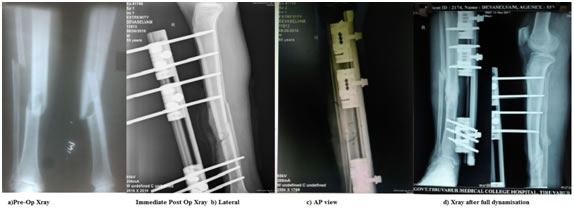
Surgical Technique All patients were operated under spinal anaesthesia. After draping the surgical site thorough wound debridement done fracture reduced and stabilised with Orthofix rail fixator with minimum of three pins on both sides of the fracture. The wound is closed in layers over suction drain. Drain removed on 2nd postoperative day. Suture is removed on 12th post operative day and discharged. Follow Up The patient is mobilised on the 2nd post operative day after drain tube removal. The patient is advised to walk without weight-bearing on the affected limb with the support of walker. Active knee and ankle mobilisation exercise were taught. The patient is advised to come for follow up every four weeks after discharge. X-Ray Leg both Antero-posterior and Lateral view were taken in every visit. The patient is advised for tip-toe walking after some period depending upon the fracture comminution, configuration and clinical finding. After adequate callus is seen the fixator is dynamized and the patient is allowed to walk without support to allow fracture consolidation. Then the patient is asked to come for follow up every 3 weeks to look for fracture consolidation both radiologically and clinically. Once fracture consolidation is achieved fixator is removed and the functional outcome is evaluated using LEFS scale. Fracture union graded radiologically by RUST score. RESULTS The severity of the fracture is graded using Gustilo-Anderson Classification. Among the 30 patients 5 (16.66%) had Gr I Compound fracture, 11 (36.66%) had Gr II fracture, 10 (33.33%) had Gr IIIA fracture and 4 (13.33%) had Gr IIIB fracture. In 17 (56.66%) patients had right leg fracture 13 (43.33%) patient had left leg fracture. 22(73.33%) patients are male 8 (36.66%) patients are female. The mean age of the study population is 43.33 years ranging from 18 to 65 years. The average follow up period is 32.26 weeks ranging from 24 to 42 weeks. The mean operating time is 48.16 minutes. The complications related to surgery are Skin Necrosis, Pin infection, Shortening. One patient (3.33%) had shortening of 2cm which is due to severe comminution. One patient (3.33%) had superficial skin infection which was treated with antibiotics. Three patients (10%) had skin necrosis and was treated with skin grafting, skin necrosis is seen in patient with Grade IIIA fracture. Six patients (20%) had pin tract infection, pin tract infection is classified into 4 grades (Tab:3), 2(6.66%) had Gr 2 infection, 4(13.33%) had Gr 1 infection. One patient required fasciotomy and later skin grafting. Three cases of Grade IIIB fractures required flap cover. One patient (3.33%) had delayed union which was treated with bone grafting and achieved fracture union. The patients during follow up were evaluated for clinical outcome, radiological fracture union and functional outcome. Clinical outcome evaluated by fracture site tenderness, Radiological progression of fracture union is measured using Radiographic Union Score for Tibial fractures score6,7 (RUST score)(Tab :2) , functional outcome is measured using Lower Extremity Function Scale (LEFS)LEFS8 is calculated with a Questionnaire containing twenty activity based questions like Any of usual work, housework or school activities, Walking between rooms, Squatting, Lifting an object from the floor, Performing light activities around home, Going up or down 10 stairs, Standing for 1 hour etc. Each were given up to 4 points adding to a maximum score of 80 and score is converted into percentage. The patients during follow up were examined clinically to check any fracture site tenderness, X-rays were taken every 4 weeks to look for callus. If there is adequate amount of callus is seen and no fracture site tenderness the fracture is consolidating. The fixator is dynamized and allowed for full weight bearing. The mean follow up period is 32.26 weeks. The average time for dynamization is 18.39 weeks, the mean time for consolidation of fracture calculated by time taken for full unsupported weight bearing i.e. mean fracture healing period is 24.39 weeks. Mean RUST score at the end of study is 2.6 out of 3. The functional outcome calculated by LEFS at the end of follow up is 88.75%.
Table 1:
Table 2: Radiographic union score for tibial (RUST) fractures
Table 3: Classification of Pin Tract Infections
DISCUSSION The management of compound fractures both initial and definitive were overcome by intramedullary nailing, but the use of improved external fixator devices like Ilizarov apparatus, Orthofix-Limb reconstruction system has made the management of compound tibia fractures more successful. Static and fatigue tests of the standard Orthofix Dynamic Axial fixator were performed to evaluate bending, torsional and axial stiffness Under similar stresses, the Orthofix device offered better torsional stiffness, higher bending stiffness in both directions and lower axial stiffness when compared to many of conventionally used external fixators9. The standard Orthofix device could be re-used, with replacing certain fixator components after inspection. The Orthofix-LRS being a stable construct giving multiplanar stability also have been designed to give compression or distraction and accurate alignment of fractures while permitting micro mobility without affecting the stability at the fracture site creating a suitable physiological condition for union at various stages of fracture healing. The timing of dynamization plays an important role in avoiding non union, malunion and implant failure as sometimes the united fibula may prevent dynamization. In our study one such case united fibula prevented dynamization which was later treated with bone grafting and fibulectomy, but achieved union at 32 weeks. For the management of the compound tibia fractures the above study shows good result which was confirmed previously by studies10. The fracture union is achieved at a mean time of 24.4 weeks which comparable to previous other studies2, 10. Six patients (20%) had pin tract infection which was unavoidable but none required pin removal. Four patients (13.33%) had Split skin grafting as second procedure of them 3 patients had Grade IIIA open fracture an skin necrosis followed after primary closure and one patient had undergone fasciotomy due to compartment syndrome then followed by SSG. Three patients (10%) had flap cover, two at initial stage and one as second procedure. All the patients had uneventful union. The Orthofix-LRS is easy and not demanding to apply. The main problem with maintaining the treatment is compliance of the patient, so proper education about duration of treatment, about postoperative rehabilitation to achieve good rate of union and functional outcome. The average functional outcome as calculated by LEFS scale is 88% ranging from 78.75% to 93.75%. One case had shortening of 2cm and had LEFS of 81.25%, shortening is due to severe comminution. The Orthofix fixator was cheaper than alternative methods in particular because no readmissions were required for implant removal.
CONCLUSION The open tibia fracture which is most common open fracture is difficult to treat due its complexity in blood supply and lack of soft tissue coverage. The study shows that the application of Orthofix fixator is less demanding than other available systems, application is straight forward and can be accomplished rapidly. Trauma during application of Orthofix produces minimal soft tissue damage and also allows adjustment of fracture reduction subsequent to application. However the outcome both functional and clinical mainly depends upon the patient aftercare and rehabilitation. Proper implementation of this unilateral frame giving multiplanar stability which can be converted into dynamic fixator combined with planned mobilisation and follow up gives good outcome. Proper timing of dynamization should be done to avoid non-union, malunion or angulations. So Orthofix fixator can be used with good results in severe open fractures. None of the authors has received or will be receiving benefits for personal and professional use from a commercial party which is related directly or indirectly to the subject of this article.
REFERENCES
|
|
 Home
Home