|
Table of Content - Volume 19 Issue 3 - September 2021
Pain score and outcome comparison between laparoscopic and open hernia surgery
Nilesh Sinha1, Shahaji Chavan2, Firoz Alam3*, Visheshta Mehan4, Vidit Puri5
1,3Assistant Professor, 2Professor & HOD, 4Student MBBS, Department of General Surgery, Dr. D Y Patil Hospital and Research centre, Pimpri, Pune Maharashtra Pincode- 411018, INDIA. 5Student MBBS, Department of Surgery, Himalayan Institute of Medical Sciences, Swami Ram Nagar,Jolly Grant, Uttarakhand. 248016, INDIA. Email: drnilu007@gmail.com, firoz10555@yahoo.com, visheshtamehan23@gmail.com, vidit.puri@gmail.com
Abstract Background: Traditional tissue repairs have stood the test of time since its inception. But for the last two decades, there has been dramatic evolution in the management of inguinal hernia with the aim to reduce post- operative pain, recurrence, and period of work loss and disability. The main objective of this project is to compare tension-free open mesh hernioplasty with total extra-peritoneal(TEP) / transabdominal pre- peritoneal(TAPP) laparoscopic hernia repair on the basis of operating time, serious intra- operative complications and the ease of tackling them, wound infection, time to return to work, chronic pain, hernia recurrence and cost implication. Design: Prospective collection of outcome data by interview of patients at day 1 and 1 week following non-randomised elective hernia repair by a single surgical group between May 2019 and September 2019. Setting: Dr. D.Y Patil Medical College and Hospital, Pimpri, Pune. Patients: A total of 50 patients (47 men; mean age, 59 years) underwent repair by laparoscopic (n = 22, 21 bilateral, 18 total extraperitoneal, and 4 transabdominal preperitoneal) or tension-free open (n = 28, 26 unilateral) approach. Laparoscopic patients were significantly younger (52.0 vs 63.8 years, P<.001). Main Outcome Measures: Subjective measures included VAS scores (1-10, 1 indicates best) for pain at 1 day and 1 week postoperatively and overall satisfaction at 1 week. Objective measures included quantity and days of analgesic use and days before return to regular activities, including work and driving. Results were also compared by patient age (Spearman analysis). Results: Satisfaction was high for both procedures; the laparoscopic procedure was superior only for return to work and driving. Spearman analysis showed a significant inverse relation between age and first-day pain (r= -0.15, P=.01), independent of operative approach. Because laparoscopic patients were younger, patients younger than 65 years were analyzed separately; laparoscopic patients had significantly less first-day pain (5.44 vs 6.30, P=.02). Conclusions: Pain following hernia repair was age dependent. Following laparoscopic repair, patients had lower first-day pain scores in younger patients and earlier return to normal activities in all patients. Satisfaction was similar for both approaches. Subjective experiences can be quantified, compared to detect subtle differences in outcome for competing surgical techniques, and used to counsel patients before operation, with the goal of improving satisfaction
INTRODUCTION "Groin hernia repair does not have the glamour of a Whipple or of a heart transplant, but in terms of preserving years of useful life, in sheer volume, is one of the most important surgical procedures." Jonathan E. Rhoades Hernias are among the oldest known afflictions of humankind and surgical repair of the inguinal hernia is the most common general surgery procedure performed today; however, the newer repair techniques continue to evolve. It is estimated that 5% of the population will develop an abdominal wall hernia, but the prevalence may be even higher. About 75% of all hernias occur in the inguinal region.1 The commonest surgery performed for inguinal hernia is the open tension-free Lichtenstein's mesh hernioplasty. It is an established fact that mesh-based repairs have a recurrence rate of 5 to 30% as opposed to primary repair sutures only with recurrence rates over and above 50%.2 After 1990, the attention was focused on the laparoscopic repair and this technique has made hernia surgery glamorous. Laparoscopic hernia repair is a relatively newer repair technique which has been widely used with an even lower recurrence rate (0-5%).3 Since the advent and wide-spread application of laparoscopy, inguinal hernia surgery received a new dimensional approach claiming equivalent or even better results than the available methodologies. The increased cost of laparoscopy was obviated by other factors like less morbidity and earlier return to work. Laparoscopic inguinal hernia repair has been tested in a number of trials but with conflicting results. Moreover, most of these trials are from the western world, which does not reflect the true picture from developing countries. The present study was designed to evaluate the effectiveness of the laparoscopic procedure compared with open mesh technique for treatment of inguinal hernia in a developing country.
METHODS Present study is a non- randomized comparative study. The study consisted 50 patients treated with hernioplasty (20 cases of laparoscopic hernioplasty and 30 cases of open hernioplasty) in the Department of General Surgery, during the study period of one year. Written consent taken from all the cases. Clearance from ethical committee of the hospital was taken for laparoscopic hernia repairs. Inclusion criteria All patients of both sex, who were 18 years of age or older with a diagnosis of inguinal hernia, either bilateral or unilateral and were medically fit to undergo the procedure were included in the study. Exclusion criteria Patients with age less than 18 years of age, contraindication to general anaesthesia (for laparoscopic repair) / Regional anaesthesia (for open repair), patients with complicated inguinal hernia like obstruction, strangulation or gangrene. Patients who have undergone previous lower abdominal surgeries. Data were collected using a questionnaire. Preoperatively the patients were offered options of either laparoscopic repair or open Lichtenstein’s repair for inguinal hernia, and were educated about the advantages, disadvantages and type of anesthesia. Preoperative evaluation of patient for laparoscopic repair includes: cardiac evaluation such as 2D ECHO if required. Pulmonary function test (PFT) for assessment of pulmonary function in some patients, and ultrasonography to rule out prostate enlargement. If the patient is not fit for general anaesthesia, laparoscopic repair is not advised, and patient is advised to go for open Lichtenstein’s repair. Operative steps and per operative complications were noted in detail and tabulated. Post-operative assessment with respect to post-operative pain, hospital stay, and other complications were included as per protocol. Patients were followed up for a period of minimum six months after surgery. That is one week after surgery, once in a month for 3 months, and once in three months thereafter. At the end of the study comparison was be made between open Lichtenstein’s repair and laparoscopic repair regarding safety and efficacy, duration of surgery with hospital stay and cost effectiveness, postoperative morbidity and patient satisfaction. Subjective data included satisfaction and pain. Patients were asked to rate (1) overall satisfaction with the operative experience on the seventh postoperative day and (2) postoperative pain on the first and seventh days. The rating tool was a VAS score with a range of 1 (best score) to 10 (worst score)2-4; patients were asked to identify the facial expression that represented their subjective experience, and the corresponding number was then recorded. Objective data included (1) quantity and duration of analgesic use and (2) the number of postoperative days before returning to regular activities in which the patients had engaged before operation. These activities included driving, work, and athletics; patients were instructed to return to these activities when they felt comfortable doing so. They were instructed not to drive or operate machinery while they were taking narcotic pain medication. Procedure details: Patients with inguinal hernia who would opt for open surgery will undergo Lichtenstein tension-free hernioplasty. During a routine traditional open surgery for hernia repair, the surgeon makes a single incision (generally 2 to 4 inches) in the groin. The protruding organ is moved back into place. The surgeon strengthens the posterior abdominal wall with synthetic mesh and closes it.[5] Patients opting for laparoscopic repair will undergo a totally extraperitoneal (TEP)/ transabdominal pre-peritoneal (TAPP) laparoscopic repair. The preperitoneal space is entered just below the umbilicus and enlarged using gentle blunt dissection with a laparoscope. Two 5-mm ports are placed in the midline under direct vision, and reusable cannulas and instruments are used. After the hernia sac is reduced, a15x10cm polypropylene mesh is used to cover the myopectineal orifice in all patients and is fixed to the pectineal ligament and further laterally using tacks. Statistical analysis Qualitative data will be expressed as percentages and proportions. Quantitative data will be expressed as mean and standard deviation. The differences between two groups with respect to continuous variables will be analysed using t-test while categorical variables will be analysed using chi-square test. All the statistical tests will be performed in SPSS version 15 software. P value <0.05 will be considered as statistically significant while P value <0.01 will be considered as statistically highly significant.
RESULTS During the study period, 97 patients underwent inguinal herniorrhaphy with mesh. Of these, 47 were excluded because of incomplete questionnaires. Consequently, 50 patients, 22 who underwent laparoscopic repair and 28 who underwent open repair, were compared in this analysis. Average age was 58.6 years (range, 20-98 years), and 47 (94%) were male. The demographics of the 47 excluded patients were similar to those included in the study. Perioperative data Patients undergoing laparoscopic repair were younger and more frequently male. Bilateral hernias were far more common in the laparoscopic group. All laparoscopic repairs required general anesthesia, whereas most open repairs were performed with the patient under local anesthesia. The principal operative technique was total extraperitoneal repair in the laparoscopic group and Lichtenstein repair in the open group. Operative times were significantly longer for laparoscopic repairs (Table 1). There were no major complications. Although the difference did not achieve significance, minor complications were more common in the laparoscopic group and included wound problems in 10 (infection, hematoma, or seroma), urinary retention in 4, and others (non– hernia-related complaints, such as dizziness, hemorrhoids, and constipation) in 5. Complications in the open repair group included wound problems in 12 and urinary retention in 1.
Table 1: Perioperative Data*
*Data are given as number (percentage)of patients excep where indicated Outcome data Overall satisfaction was similarly high for both laparoscopic and open procedures. Pain scores decreased significantly from the first to the seventh postoperative day, but there were no differences between groups (Table 2). Pain scores are shown in Figure 1; the distribution of scores was broad at 1 day and much narrower at 1 week following operation. Analgesic requirements, both quantity and duration, were similar for both groups. Following the laparoscopic procedure when compared with open repair, patients returned earlier to driving and work but not athletics.
Table 2: Outcome Data foe all Patients*
*Data are given as mean SD except where indicated
Table 3: Outcome Data foe all Patients Younger than 65 Years*
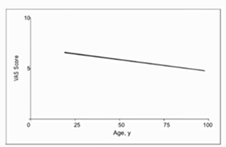
*Data are given as mean SD except where indicated Analysis by age When data were analyzed using Spearman rank order correlation (Figure 2), there was a significant inverse relation between age and pain score on the first postoperative day (r = −0.15, P = .02), with younger patients having higher overall scores. Although statistically significant, age accounts for only a small amount (2%) of the variability in first-day pain. Because patients undergoing laparoscopic repair were significantly younger than those who underwent open repair, outcome data were also analyzed for patients younger than 65 years. In contrast to the entire series, younger patients who underwent laparoscopic repair had lower pain scores on the first postoperative day when compared with younger patients who underwent open repairs. However, there was no difference by the seventh postoperative day.
DISCUSSION Successful hernia treatment should offer high patient satisfaction, low cost, low recurrence rate, and rapid return to work.7 Laparoscopic and open hernia repairs fulfil this criterion8 However, the question about the most appropriate technique still confuses the community of surgeons. Several studies have compared the laparoscopic and open techniques for inguinal hernia repair. The advantages of laparoscopic hernia repair over traditional open repair in terms of limited post-operative pain, shorter hospitalisation, early resumption of activity and improved cosmetic have been readily apparent and accepted. Despite excellent long-term outcome after TAPP repair, the use of laparoscopy in hernia repair is still limited. Our data show that patient satisfaction and subjective pain can be quantitated and that these are similar for laparoscopic and tension-free open hernia repair when performed in selected patients. Satisfaction was high for both procedures. Pain scores decreased significantly from the first to seventh postoperative day. After laparoscopic repair, patients returned earlier to work and driving. Patients younger than 65 years experienced more pain than those 65 years and older. Younger patients had less pain with laparoscopic than with open repair, even though most underwent bilateral laparoscopic herniorrhaphies. The number of days before returning to work and driving was significantly shorter in the laparoscopic group, but the laparoscopic patients were younger, and socioeconomic factors, which have been shown to influence return to work, were not studied. The age difference may also have affected the time to return to driving, which was shorter in the laparoscopic patients. However, when patients younger than 65 years were analyzed separately, there was no difference in return to driving. Overall satisfaction, which reflects the entire operative and perioperative experience, is of great importance but difficult to quantitate. Satisfaction is most often measured by adjectives ("very satisfied," "moderately satisfied," or "dissatisfied"); these terms have been used to compare satisfaction data for laparoscopic vs open hernia repair.11-13 Our data were collected by showing the patients a VAS and asking them to point to a face that corresponds with their level of satisfaction with the procedure. The patients readily identify the appropriate face, requiring less reasoning and rationalizing than a numerical scale. Many factors affect pain, including type of operation, complications, age, tolerance, and cultural issues. Different anesthetic techniques also may affect postoperative pain. In our series, all patients in the laparoscopic group had general anesthesia, whereas most patients in the open group had local anesthesia. Of note, a randomized trial that compared local with general anesthesia in open hernia repair showed no difference in postoperative pain or recovery.14 The VAS score is superior because of its documented reliability and validity. It has been proven to be a linear scale for quantifying pain and to be accurate for serial measurements.2,3 Additionally, the absolute values of VAS measurements are clinically relevant. Most agree that VAS scores from 0 to 3 correspond to mild pain, for which patients do not seek analgesia. Scores from 4 to 6 represent moderate pain and 7 to 10 severe pain. When analyzing data in these broad categories, it is possible to identify clinically significant differences between treatment groups. In the moderate or severe ranges, several studies show clinical significance if the difference in pain score is at least 0.9 or 1.3 between groups. Several investigators have used pain assessment by VAS to compare hernia techniques. The pain scores on postoperative day 1 ranged from 1.8 to 5.4 for laparoscopic repairs and 2.2 to 5.7 for open repairs. The variability of scores emphasizes the uniqueness of patient populations, but the differences in scores between techniques in each study were similar: 0.3 to 1.9 (postoperative day 1) and 0.1 to 1.5 (day 7). The difference in pain scores on the first postoperative day between laparoscopic and open technique in our patients younger than 65 years was 0.9 and was statistically significant. Calculated difference in scores is a useful comparative tool, using VAS for baseline scoring, because VAS is a simple and uniformly accepted method to assess pain and is used in most hospitals. A thorough knowledge of the anatomy and the operative approach, along with advanced laparoscopic skills will reduce the possibility of significant complications. With experience and technical improvements, the complications are now minimal in the laparoscopic repair and studies indicate similar complication rates between open and laparoscopic repairs. In the present study, the mean post-operative hospital stay was 2.6 days for laparoscopic hernia repair group, whereas it was 6.1 days for Open Lichtenstein’s repair.Hence the mean post-operative hospital stay was significantly less in laparoscopic repair than open hernia repair with p<0.0001 which was extremely significant. So, from this study it can be concluded that laparoscopic hernia repair is associated with less postoperative hospital stay and better comfort than open hernia repair. Studies state that patients have a shorter convalescence and a faster return to work and activities after laparoscopic repair compared to open mesh repair. Data regarding time to return to activity are rather subjective. Type of employment or profession, to which patient is returning will influence how long he needs to be away from work. Patient who is doing desk job in office will return to work earlier than a patent with a job that entails heavy lifting. In the present study patients who underwent laparoscopic hernia repair were able to return to their normal work earlier in a mean period of 8.73 days than those patients who underwent open repair returned to their normal work in a mean period of 11.29 days with p<0.001 which is extremely significant. This is a great advantage for Indian patients particularly who attend government hospital like ours who earn livelihood on a day to day basis. Most studies mentioned early return to normal work as an advantage of laparoscopic hernia repair, which has been repeated in this study. However, as mentioned, there might not be any difference between the two groups in the level of activity on long-term follow up. One of the major criticisms of laparoscopic hernia repair is that it is more expensive to perform than open hernia repair. The primary reason for this relates to the cost of extra equipment used for the laparoscopic repair with secondary costs attributed to perceived increases in operating time for the laparoscopic procedure.
CONCLUSION Inguinal hernia is a common problem, which can be treated only by surgery. The results support the view that laparoscopic pre-peritoneal mesh repair is safe and efficient when compared to open mesh repair of inguinal hernia. There is definitive learning curve for surgeons who are newly exposed. The complication rate reduces as the surgeons become more experienced in this procedure comparable with that of open repair. Laparoscopic pre- peritoneal mesh repair is safe with less post-operative morbidity associated with faster recovery and satisfaction as documented by less post- operative pain, earlier mobilization and discharge from the hospital, as well as early return to work. The hard working below poverty people should be given best treatment, which should allow them to go for their regular work at the earliest and with complete integrity. As it is costly in private hospitals, the faculty of government hospitals should cater the best treatment at free of cost for poor. To achieve this goal the surgeons should improvise their technical skills in laparoscopic repair of inguinal hernia (TAPP and TEP) with short learning curve. The present study supports the view that laparoscopic pre- peritoneal mesh repair of inguinal hernia is safe and efficacious and offers definitive advantages over open mesh repair and should be an available option for all patients requiring elective hernioplasty.
REFERENCES
Policy for Articles with Open Access
|
|
 Home
Home